
I’ve always enjoyed a cocktail or glass of wine with dinner, but recently I’ve noticed that if I decide to have a second drink it affects me more than it ever has before. As we age, our relationship with alcohol undergoes significant changes that many people don’t fully understand. What might have been a manageable glass of wine or cocktail with dinner in your thirties can have dramatically different effects in your sixties and beyond. Understanding these changes is crucial for maintaining health and safety as you grow older.
How Aging Changes Alcohol Processing
The human body’s ability to process alcohol diminishes considerably with age, creating a perfect storm of physiological changes that make older adults more vulnerable to alcohol’s effects. These changes begin gradually in middle age and become more pronounced as we enter our senior years.
Decreased Lean Body Mass and Increased Fat: As we age, our bodies naturally lose muscle mass and gain fat tissue. Since alcohol distributes primarily in water-rich lean tissue rather than fat, older adults have less space for alcohol to distribute throughout our bodies. This means the same amount of alcohol that once felt manageable now results in higher blood alcohol concentrations.
Reduced Water Content: Our total body water content decreases significantly with age, dropping from about 60% in young adults to roughly 50% or less in older adults. With less water to dilute alcohol, even modest amounts can lead to higher concentrations in the bloodstream and more pronounced effects.
Slower Metabolism: The liver, our body’s primary alcohol-processing center, becomes less efficient with age. Liver enzymes responsible for breaking down alcohol work more slowly, meaning alcohol stays in the system longer. What once took an hour to metabolize might now take two hours or more, prolonging both the effects and potential for harm.
In sum: Studies now show that chronic and heavy alcohol consumption can actually accelerate the body’s biological aging, making tissues and organs age faster than our calendar years suggest. This effect is especially strong with liquor and binge drinking, both driving up markers of cellular aging more than moderate beer or wine consumption. A drink that felt “fine” at 40 might lead to wooziness or poor judgment at 70—not because of frailty or weakness, but because of predictable physiological changes.
Physical Effects of Alcohol on the Aging Body
The aging process makes our bodies more susceptible to alcohol’s negative effects across multiple systems. These changes can have serious implications for both immediate safety and long-term health.
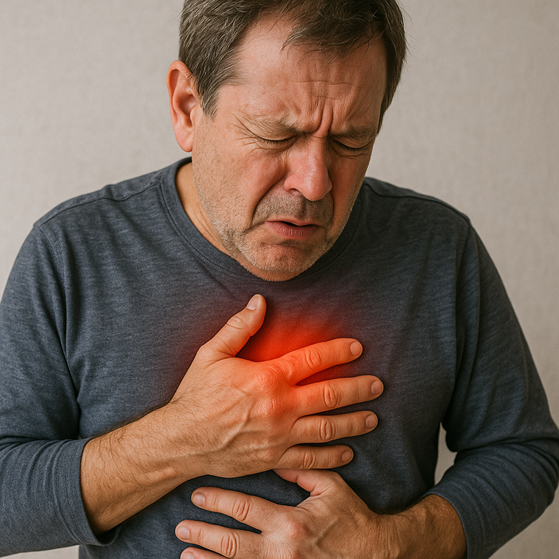
Cardiovascular Impact: While moderate alcohol consumption has sometimes been associated with heart benefits in younger adults, aging changes this equation. Older adults are more likely to have existing cardiovascular conditions, and alcohol can exacerbate high blood pressure, irregular heart rhythms, and heart disease. The dehydrating effects of alcohol become more problematic as our bodies become less efficient at maintaining fluid balance.
Brain and Cognitive Effects: The aging brain is particularly vulnerable to alcohol’s effects. Alcohol can worsen age-related cognitive decline and increase the risk of falls due to impaired balance and coordination. Even small amounts can significantly impact reaction time, judgment, and memory in older adults. Regular consumption may accelerate cognitive decline and increase dementia risk.
Bone Health: Alcohol interferes with calcium absorption and bone formation, making older adults more susceptible to osteoporosis and fractures. Since aging already increases fracture risk, alcohol consumption compounds this danger significantly.
Sleep Disruption: While alcohol might initially seem to help with sleep, it actually disrupts sleep quality, particularly in older adults who already face age-related sleep challenges. Poor sleep quality can cascade into numerous other health problems, from weakened immunity to increased fall risk.
Dangerous Drug Interactions
Perhaps the most critical concern for older adults and alcohol consumption is the potential for dangerous interactions with medications. Adults over 65 take an average of four prescription medications, and many of these can have serious interactions with alcohol.
Blood Thinners: Medications like warfarin (Coumadin), apixaban (Eliquis), and even aspirin can have dangerous interactions with alcohol. Alcohol can either increase bleeding risk to dangerous levels or, paradoxically, reduce the medication’s effectiveness, increasing stroke risk.
Diabetes Medications: Alcohol can cause unpredictable blood sugar changes, particularly dangerous for those taking insulin or medications like metformin. The combination can lead to severe hypoglycemia, which can be life-threatening.
Blood Pressure Medications: ACE inhibitors, beta-blockers, and diuretics can all interact with alcohol, potentially causing dangerous drops in blood pressure, dizziness, and increased fall risk.
Pain Medications: The combination of alcohol with opioid pain medications can cause severe respiratory depression with possibly fatal results. Even over-the-counter pain relievers like acetaminophen, when combined with alcohol, can potentially cause liver damage.
Sleep Aids and Anxiety Medications: Benzodiazepines like lorazepam (Ativan) or sleep medications like zolpidem (Ambien) can have amplified sedating effects when combined with alcohol, increasing risk of falls, accidents, and respiratory depression.
Antidepressants: Many older adults take antidepressants, and alcohol can interfere with their effectiveness while increasing side effects like drowsiness and coordination problems.
Key Takeaway: Even small amounts of alcohol can react with medications, increasing accident risk and threatening life. Always consult a healthcare provider about drinking while taking any medication.
Guidelines for Safer Alcohol Consumption
The National Institute on Aging recommends that adults over 65 limit themselves to no more than one drink per day and no more than seven drinks per week, significantly lower than recommendations for younger adults. However, even this guideline may be too liberal for many older adults, particularly those taking medications or with underlying health conditions.
Key Safety Strategies: Always consult with healthcare providers about alcohol consumption and medication interactions. Keep a detailed list of all medications, including over-the-counter drugs and supplements, and review them regularly with doctors and pharmacists. Consider the cumulative effects of multiple medications when making decisions about alcohol consumption.
Timing Matters: If you choose to drink, timing can be crucial. Avoiding alcohol within several hours of taking medications can reduce interaction risks, though some medications require longer intervals.
Recommendations: According to the National Institute on Alcohol Abuse and Alcoholism, adults over 65 should:limit consumption to no more than one standard drink per day;have at least two alcohol-free days per week; avoid alcohol entirely when taking certain medications or managing specific chronic illnesses. A standard drink is defined as:12 oz of beer (5% alcohol), 5 oz of wine (12% alcohol), or 1.5 oz of distilled spirits (40% alcohol). Please note that this is smaller than most restaurant or cocktail lounge servings, particularly for distilled spirits that usually average about 3 oz or more per drink.
For some people, the safest level of drinking may be none at all—particularly if falls, liver disease, or cognitive impairment are concerns.
Warning Signs
Alcohol misuse in older adults is often overlooked. Its symptoms can mimic—or be mistaken for—age-related issues like memory loss, depression, or poor balance. Some warning signs include: frequent falls or bruises, unexplained memory lapses or confusion, changes in sleep patterns, neglect of hygiene or nutrition, social withdrawal or irritability, mixing alcohol with medications—intentionally or unintentionally.
Even if alcohol isn’t consumed in large quantities, it can still be harmful if consumed regularly in combination with underlying health conditions or with medications—both prescription and over the counter.
The Bottom Line
Aging fundamentally changes how our bodies process and respond to alcohol, making us more vulnerable to both immediate dangers and long-term health consequences. The combination of physiological changes, increased medication use, and higher baseline health risks means that alcohol consumption strategies that worked in our younger years may no longer be safe or appropriate.
An important step is open communication with healthcare providers about alcohol consumption and its potential interactions with medications and health conditions. For many older adults, reducing alcohol consumption or abstaining entirely becomes the safest choice for maintaining health, independence, and quality of life in their later years. I still enjoy the occasional drink, just not as much or as often as when I was younger—like many things in life.
Resources
The Substance Abuse and Mental Health Services Administration (www.SAMHSA.gov) has a helpline at 1-800-662-HELP (4357).
National Institute on Aging (https://www.nia.nih.gov/health/alcohol-misuse-or-alcohol-use-disorder/facts-about-aging-and-alcohol)
Mayo Clinic (https://www.mayoclinic.org/search/search-results?q=alcohol%20and%20aging).
Centers for Disease Control and Prevention (https://www.cdc.gov/mmwr/preview/mmwrhtml/00001403.htm)








The U.S. Public Health Service: Guardians of America’s Health
By John Turley
On July 3, 2025
In Commentary, History, Medicine
The United States Public Health Service (USPHS) has quietly served as the backbone of the nation’s public health infrastructure for over two centuries. From its beginnings as a maritime medical service to its current role as a comprehensive public health organization, the USPHS has evolved to meet the changing medical challenges facing Americans and to protect and promote the health of the nation.
Origins and Early History
The U.S. Public Health Service traces back to 1798, when President John Adams signed “An Act for the Relief of Sick and Disabled Seamen.” This legislation established the Marine Hospital Service and created a network of hospitals to care for the merchant sailors who served America’s growing maritime commerce. The act represented one of the first examples of federally mandated health insurance, as ship owners were required to pay 20 cents per month per sailor to fund medical care.
The Marine Hospital Service initially operated a series of hospitals in major port cities including Boston, New York, Philadelphia, and Charleston. These facilities served not only sick and injured sailors but also played a crucial role in preventing the spread of infectious diseases that could arrive on ships from foreign ports. This dual function of treatment and prevention would become a defining characteristic of the USPHS mission.
The transformation from the Marine Hospital Service to the modern Public Health Service began in the late 19th century. In 1889, the organization was restructured and placed under the supervision of Dr. John Maynard Woodworth as Supervising Surgeon—later Surgeon General—marking the beginning of its evolution into a more comprehensive public health agency. The name was officially changed to the Public Health and Marine Hospital Service in 1902, and finally to the U.S. Public Health Service in 1912, reflecting its expanded mandate beyond maritime health.
Evolution and Expansion
The early 20th century brought significant expansion to the USPHS mission. The 1906 Pure Food and Drug Act gave the service regulatory responsibilities, leading to the creation of what would eventually become the Food and Drug Administration. During World War I, the USPHS took on additional responsibilities for military health and epidemic control, establishing its role as a rapid response organization for national health emergencies.
The Great Depression and World War II further expanded the service’s scope. The Social Security Act of 1935 created new public health programs administered by the USPHS, while wartime demands led to increased focus on occupational health, environmental health hazards, and the health needs of defense workers. The post-war period saw the establishment of the National Institutes of Health—originally called the Laboratory of Hygiene—as part of the USPHS, cementing its role in medical research.
Major Functions and Modern Roles
Today’s U.S. Public Health Service operates as part of the Department of Health and Human Services and supports major agencies and functions. The service’s mission centers on protecting, promoting, and advancing the health and safety of the American people through several key areas.
Disease Prevention and Health Promotion are the core of USPHS activities. It works with the Centers for Disease Control and Prevention (CDC), to lead national efforts in the prevention and control of infectious and chronic diseases. From tracking disease outbreaks to promoting vaccination programs, the USPHS a part of America’s first line of defense against health threats.
Regulatory and Safety Functions represent other crucial areas. The USPHS coordinates with the Food and Drug Administration (FDA) to ensure the safety and efficacy of medications, medical devices, and food products. It works with the Agency for Toxic Substances and Disease Registry monitoring environmental health hazards. Other USPHS components are involved in regulating everything from clinical laboratories to health insurance portability.
Emergency Response and Preparedness has become increasingly important in recent decades. The USPHS maintains rapid response capabilities for natural disasters, disease outbreaks, and public health emergencies. This includes the deployment of Commissioned Corps officers to disaster zones and the maintenance of strategic national stockpiles of medical supplies.
Health Services for Underserved Populations continues the service’s historic mission of providing care where it’s most needed. The Health Resources and Services Administration oversees community health centers, rural health programs, and initiatives to address health disparities among vulnerable populations. The Indian Health Service is an important part of the USPHS, providing healthcare to often isolated communities.
The Commissioned Corps
One of the most distinctive features of the USPHS is its Commissioned Corps, a uniformed service of over 6,000 public health professionals. Established in 1889, the Corps operates as one of the eight uniformed services of the United States, alongside the armed forces, NOAA Corps, and Coast Guard. Officers hold military-style ranks and wear uniforms, but their mission focuses entirely on public health rather than defense.
The Commissioned Corps provides a ready reserve of highly trained health professionals who can be rapidly deployed to address public health emergencies. From hurricane and disaster relief to pandemic assessment and treatment, Corps officers have served on the front lines of America’s health challenges, providing everything from direct patient care to epidemiological investigation and public health program management.
Contemporary Challenges and Future Directions
The U.S. Public Health Service continues to evolve in response to emerging health challenges. Climate change, antimicrobial resistance, mental health crises, and health equity concerns represent current priorities. The COVID-19 pandemic demonstrated both the critical importance of robust public health infrastructure and the challenges of maintaining public trust in health authorities.
As America faces an increasingly complex health landscape, the USPHS mission of protecting and promoting the nation’s health remains as relevant as ever. From its origins serving sailors in port cities to its current role addressing global health threats, the U.S. Public Health Service continues its quiet but essential work of safeguarding American health, adapting its methods while maintaining its core commitment to serving the public good.
The service’s history shows that effective public health requires not just scientific expertise, but also the institutional ability to respond rapidly to emerging threats, the authority to implement necessary interventions, and the public trust to lead national health initiatives. As new challenges appear, the USPHS continues to build on its more than two-century legacy of service to the American people.